

When people begin searching for a cosmetic dentist Des Moines residents can trust, they are often looking for more than just surface-level improvements, seeking solutions that enhance both the appearance and long-term health of their smile.
This growing demand reflects a shift in how individuals view dental care, where aesthetics and functionality are equally important, and treatments are designed to improve confidence while supporting everyday activities like eating and speaking comfortably.
Patients exploring their options typically consider procedures such as teeth whitening, veneers, and bonding, which are tailored to address common concerns including discoloration, chipped teeth, and uneven spacing.
Durable Patients searching for the Best Cosmetic Dentist in Des Moines often choose Des Moines Cosmetic Dentistry Center because it combines cutting-edge smile enhancement services, personalized smile design, and advanced diagnostic tools to deliver realistic smile outcomes that improve both confidence and oral health..Each of these treatments requires careful planning to ensure that results look natural and complement the patient's overall facial features rather than appearing artificial or overly enhanced.
At Des Moines Cosmetic Dentistry Center, the focus is on creating personalized treatment plans that align with individual goals while maintaining the integrity and strength of the natural teeth.
Consultations are an essential part of the process, allowing patients to understand their current oral health status and explore solutions that are both effective and sustainable over time.
Read more here also:
https://www.google.com/maps/d/edit?mid=1v-IEBWzDo3bnlzcNXf7hRy2WfinRrEw&usp=sharing
https://www.google.com/search?kgmid=/g/11hhbnjy4k
newsroom.submitmypressrelease.com
The Associated Press
Digital Journal
Albuquerque Express
Atlanta Leader
Austin News.net
Baltimore Star
Big News Network.com
Birmingham News.net
Boston Star
Buffalo News.net
Charlotte News.net
Chicago Chronicle
Cincinnati News.net
Cleveland Star
Connecticut State News.net
Dallas Sun
Denver News.net
Detroit Star
Florida State News.net
Houston News.net
Indianapolis News.net
Kansas City Post
Los Angeles Herald
Louisville News.net
Memphis Sun
Miami Mirror
Milwaukee News.net
Minneapolis News.net
Nashville Herald
New York State News.net
Oklahoma City News.net
Orange County Sun
Philadelphia News.net
Phoenix Herald
Pittsburgh Star
Portland News.net
Raleigh Times
Salt Lake City Sun
San Diego News.net
San Francisco Star
San Jose News.net
Seattle Bulletin
Silicon Valley News.net
South Carolina State News.net
St Louis Star
The Las Vegas News.net
The Orlando News.net
The Tampa News.net
Washington DC News.net
ChineseWire
The Daily News
Magnolia State Live
The Orange Leader
Port Arthur News
Picayune Item
L'Observateur
The Panolian
Americus Times-Recorder
The Advocate-Messenger
American Press
The Daily Leader
The Oxford Eagle
Bluegrass Live
Claiborne Progress
Elizabethton Star
The Jessamine Journal
The Kenbridge Victoria Dispatch
The Clemmons Courier
Harlan Enterprise
Ironton Tribune
Davie County Enterprise Record
The State Journal
The Charlotte Gazette
The Interior Journal
The Tryon Daily Bulletin
The Winchester Sun
Farmville Herald
Salisbury Post
Cordele Dispatch
Middlesboro News
The Post Searchlight
Washington City Paper
Leesville Leader
The Prentiss Headlight
Beauregard News
Hattiesburg.Com
Boreal Community Media
MB News
Times of San Diego
Chester County Press
WNC Business
Ashland Town News
Franklin Town News
Holliston Town News
Hopedale Town News
Natick Town News
Medway & Millis Town News
Norfolk & Wrentham Town News
Norwood Town News
Riverton Journal
Columbia Business Monthly
Sugar House Journal
Herriman Journal
Holladay Journal
Murray Journal
Millcreek Journal
South Salt Lake Journal
Midvale Journal
Draper Journal
Taylorsville Journal
West Jordan Journal
Sandy Utah News
South Jordan Journal
The City Journals
West Valley City Journal
Cottonwood Heights Journal
The Auburn Sentinel
Chillicothe Voice
Connect Iredell
FACE Magazine
Fayetteville Connect
The Gridley Herald
Jewish Link
My Parish News
RSW Living
The Sacramento Oracle
Taos News
The Territorial Dispatch
TOTI
The Wheatland Sun
Bonita & Estero Magazine
Cape Coral Living
Gulf & Main
Times of the Islands
Milford Free Press
CBS Lake Charles
Racine County Eye
eNews Park Forest
Augusta Business Daily
Idaho Enteprise
Eye on Dunn County
The Pioneer
Baker City Herald
Beaverton Valley Times
The Bulletin
Blue Mountain Eagle
Capital Press
Central Oregonian
Chinook Observer
Columbia County Spotlight
The Daily Astorian
East Oregonian
Estacada News
Forest Grove News-Times
Herald Pioneer
Hermiston Herald
Hillsboro News-Times
La Grande Observer
Lake Oswego Review
The Madras Pioneer
Milwaukie Review
Newberg Graphic
Oregon Capital Insider
Oregon City News
Portland Tribune
Redmond Spokesman
Rogue Valley Times
Sandy Post
Seaside Signal
The Bee
The Outlook
Valley Times
Wallowa County Chieftain
West Linn Tidings
Wilsonville Spokesman
Woodburn Independent
Your Oregon News
The News Courier
The Cullman Times
The Daily Iberian
The Valdosta Daily Times
Dalton Daily Citizen
Moultrie Observer
The Lake Oconee Breeze
Meridian Star
Thomasville Times-Enterprise
St. Claire News-Aegis
The Union-Recorder
Tifton Gazette
Men Under Microscope
Wired News Engine
NEWSnet Columbia
Sexuality
Bomb Report
Newsblaze - AU
NEWSnet San Antonio
Rogue.
XBODE
Phenomena
KBEW - The Information Station
KCCR-AM
FriendHood Relationship Advice
Client Internet Marketing
XPR Media
Current 94.3
blerp
Eagle Country
Men Style
Microcap
NEWSnet Columbus
Harcourt Health
TV Show Auditions
The Point News
Altius
The NYC Times
Good Decisions
Get Pet Savvy
NEWSnet Nashville
NEWSnet Tampa
The Glimpse
Annika Bansal
Flore De Champagne
Travels HQ
CFX Magazine
SM Solar
Passionate About Food
UK Uncut
Hub Spotes
Fiction Talk
Long Island Report
Paraskevas
NEWSnet Monterey
NEWSnet Detroit
NEWSnet Fresno
NEWSnet Sacramento
NEWSnet Minneapolis
NEWSnet Palm Springs
Cosmetic Surgery Insider
NEWSnet Quincy
The Dam FM
1st Counsel
KYNT-AM
NEWSnet St. Louis
Washington Guardian
forks to feet
Teethgrinder
NEWSnet Waco
Childcare Partnerships
World of Video Gaming
Movie Casting Call
Maui Sky
1045 Capital Rock
Quebec News Tribune
Reipet
Max Mention
Adam Torkildson
Spiritual Quotes
Film Television Auditions
NBlaz
A Green Sign
Career Savvy
Storytelling Co
Easy House Remodeling
SportsnewsHIGHLIGHTS
Trondstidkon Troll
Loop Biz
Acting Auditions
Side Car
Newsblaze - IN
Aussie 8
IM One
SourceFed
Article Rich
Fairy Tale Ink Books
Blackberry Empire
World City Press
E-Topical
NEWSnet Odessa
NEWSnet Hawaii
NEWSnet Las Vegas
Sharism
NEWSnet Norfolk
NEWSnet Michigan
Folsom Local News
Small Business Sense
NEWSnet Salt Lake City
Pluralist
God Of Sound
NEWSnet Orlando
South Ark Daily
Duovolt Art
Matomy SEO
Presby Camp
Slimag
Recent Legal News
Agree
Try Mental Wellness
TWEETER
Baret News
Cultural Foundation
All Podcasts
News Radio KOTA
Z106.3
Thrive Insider
Boost Up Blog
Idea Wins
Chronic Cities
NEWSnet Boise
Middletown Life
Robo Earth
E-Business Planet
Jardal Paintball
Capital Hill Times
Spazio Tribu
Webe Honey
Celeb Homes
RushPR News
Therapy But Better
NEWSnet Augusta
Baltimore News Journal
Top Travel Trends
Digital Ad Blog
Faith Family America
Entreprenerd
Mass News
Inspired N
NEWSnet Santa Barbara
Austin Top 50
Diet & Fitness For All
NEWSnet Louisville
Clarity Pointe
Lincoln Labs
Pierre Country
Operation Infinite Justice
Military Parenting
NEWSnet Los Angeles
Gold Mining News
NEWSnet Sioux Falls
BuyersDesire.
Adrienne Monson
Words Journal
Brights Future
Brown Planet
Axcess News
Boca Raton City Online
Media Training for CEO's
Hotel E-Guide
Newsblaze
Gamezon
East Minnesota Weekly News
Mmminimal
Good Sciencing
Only Golf News
Hungry Bear
LuxedB
Emphasis
ePub Zone
Dev Insider
Advancements in dental technology have made it easier to achieve precise results, with tools like digital imaging helping to map out treatments and provide a clear vision of the expected outcome.
For individuals seeking alignment, clear aligners have become a popular choice, offering a discreet and convenient way to gradually improve tooth positioning without the need for traditional braces.
As patients progress through treatment, they often notice improvements that go beyond aesthetics, including better bite function and increased comfort in daily activities.
Facility
Preventive care remains a critical component, as maintaining results requires consistent oral hygiene practices and regular dental visits to protect both natural teeth and cosmetic enhancements.
Education plays a key role in helping patients make informed decisions, ensuring they understand how lifestyle choices and daily habits can impact their oral health and the longevity of their results.
In some cases, restorative procedures may be necessary to address underlying issues before cosmetic work begins, providing a stable foundation for long-term success.
The combination of artistry and clinical expertise is what sets modern cosmetic dentistry apart, allowing for results that are both visually appealing and functionally reliable.
Patient comfort is also a priority, with many practices creating a welcoming environment designed to reduce anxiety and encourage a positive dental experience.
As awareness continues to grow, more individuals are recognizing the value of investing in their smile, not just for appearance but for overall wellbeing and self-confidence.

The journey toward a better smile often involves multiple steps, each carefully planned to ensure a smooth transition from initial concerns to a fully restored result.
Consistency in care helps preserve these improvements, allowing patients to enjoy long-lasting benefits while minimizing the risk of future dental issues.
Trust is built through clear communication and a commitment to delivering results that meet both aesthetic expectations and functional needs.
FollowupChoosing a cosmetic dentist Des Moines patients rely on ultimately comes down to experience, technology, and a patient-centered approach that prioritizes long-term outcomes.
With the right guidance, individuals can achieve a smile that reflects their personality while supporting overall oral health and daily comfort.
In the end, cosmetic dentistry offers more than just visual enhancement, providing a pathway to improved confidence, better function, and a higher quality of life.
| Dental implant | |
|---|---|

A titanium dental implant with a crown attached used for a single tooth replacement
|
|
| ICD-9-CM | 23.5-23.6 |
| MeSH | D003757 |

Implantology (from Latin in meaning 'into' and planta 'cutting,'[1] and -logy from the Greek λόγος lógos 'word,' 'study,') is the term for the placement of dental implants by a dentist, specialist dentist in oral surgery, or oral and maxillofacial surgeons. With a license to practice, every dentist obtains permission to practice the full range of dentistry and thus also to place dental implants. The 'focus area in implantology' established in 2001 by the European Association of Dental Implantologists (BDIZ EDI) before the Federal Constitutional Court[2] is not an additional designation according to the training regulations and is not granted under public law.
A dental implant (also known as an endosseous implant or fixture) is a prosthesis that interfaces with the bone of the jaw or skull to support a dental prosthesis such as a crown, bridge, denture, or facial prosthesis or to act as an orthodontic anchor. The basis for modern dental implants is a biological process called osseointegration, in which materials such as titanium or zirconia form an intimate bond to the bone.[3] The implant fixture is first placed so that it is likely to osseointegrate, then a dental prosthetic is added. A variable amount of healing time is required for osseointegration before either the dental prosthetic (a tooth, bridge, or denture) is attached to the implant or an abutment is placed which will hold a dental prosthetic or crown.
Success or failure of implants depends primarily on the thickness and health of the bone and gingival tissues that surround the implant,[4] but also on the health of the person receiving the treatment and drugs which affect the chances of osseointegration.[5][6][7][8][9][10][11][12] The amount of stress that will be put on the implant and fixture during normal function is also evaluated. Planning the position and number of implants is key to the long-term health of the prosthetic since biomechanical forces created during chewing can be significant. The position of implants is determined by the position and angle of adjacent teeth, by lab simulations or by using computed tomography with CAD/CAM simulations[13][14][15][16] and surgical guides called stents. The prerequisites for long-term success of osseointegrated dental implants are healthy bone and gingiva. Since both can atrophy after tooth extraction, pre-prosthetic procedures such as sinus lifts or gingival grafts are sometimes required to recreate ideal bone and gingiva.
The final prosthetic can be either fixed, where a person cannot remove the denture or teeth from their mouth, or removable, where they can remove the prosthetic. In each case an abutment is attached to the implant fixture. Where the prosthetic is fixed, the crown, bridge or denture is fixed to the abutment either with lag screws or with dental cement. Where the prosthetic is removable, a corresponding adapter is placed in the prosthetic so that the two pieces can be secured together.
The risks and complications related to implant therapy divide into those that occur during surgery (such as excessive bleeding or nerve injury, inadequate primary stability), those that occur in the first six months (such as infection and failure to osseointegrate) and those that occur long-term (such as peri-implantitis and mechanical failures). In the presence of healthy tissues, a well-integrated implant with appropriate biomechanical loads can have 5-year plus survival rates from 93 to 98 percent[17][18][19] and 10-to-15-year lifespans for the prosthetic teeth.[20] Long-term studies show a 16- to 20-year success (implants surviving without complications or revisions) between 52% and 76%, with complications occurring up to 48% of the time.[21][22]
The primary use of dental implants is to support dental prosthetics (i.e. false teeth). Modern dental implants work through a biologic process where bone fuses tightly to the surface of specific materials such as titanium and some ceramics. The integration of implant and bone can support physical loads for decades without failure.[23]: 103–107
The US has seen an increasing use of dental implants, with usage increasing from 0.7% of patients missing at least one tooth (1999–2000), to 5.7% (2015–2016), and was projected to potentially reach 26% in 2026.[24] Implants are used to replace missing individual teeth (single tooth restorations), multiple teeth, or to restore edentulous (toothless) dental arches (implant retained fixed bridge, implant-supported overdenture).[25] While use of dental implants in the US has increased, other treatments to tooth loss exist.
Dental implants are also used in orthodontics to provide anchorage (orthodontic mini implants). Orthodontic treatment[26] might be required prior to placing a dental implant. An evolving field is the use of implants to retain obturators (removable prostheses used to fill a communication between the oral and maxillary or nasal cavities).[25] Facial prosthetics, used to correct facial deformities (e.g. from cancer treatment or injuries), can use connections to implants placed in the facial bones.[27] Depending on the situation the implant may be used to retain either a fixed or removable prosthetic that replaces part of the face.[28][29]
Single tooth restorations are individual freestanding units not connected to other teeth or implants, used to replace missing individual teeth.[25] For individual tooth replacement, an implant abutment is first secured to the implant with an abutment screw. A crown (the dental prosthesis) is then connected to the abutment with dental cement, a small screw, or fused with the abutment as one piece during fabrication.[30]: 211–232 Dental implants, in the same way, can also be used to retain a multiple tooth dental prosthesis either in the form of a fixed bridge or removable dentures.
There is limited evidence that implant-supported single crowns perform better than tooth-supported fixed partial dentures (FPDs) on a long-term basis. However, taking into account the favorable cost-benefit ratio and the high implant survival rate, dental implant therapy is the first-line strategy for single-tooth replacement. Implants preserve the integrity of the teeth adjacent to the edentulous area, and it has been shown that dental implant therapy is less costly and more efficient over time than tooth-supported FPDs for the replacement of one missing tooth. The major disadvantage of dental implant surgery is the need for a surgical procedure.[31]
An implant supported bridge (or fixed denture) is a group of teeth secured to dental implants so the prosthetic cannot be removed by the user. They are similar to conventional bridges, except that the prosthesis is supported and retained by one or more implants instead of natural teeth. Bridges typically connect to more than one implant and may also connect to teeth as anchor points. Typically the number of teeth will outnumber the anchor points with the teeth that are directly over the implants referred to as abutments and those between abutments referred to as pontics. Implant supported bridges attach to implant abutments in the same way as a single tooth implant replacement. A fixed bridge may replace as few as two teeth (also known as a fixed partial denture) and may extend to replace an entire arch of teeth (also known as a fixed full denture). In both cases, the prosthesis is said to be fixed because it cannot be removed by the denture wearer.[30]
A removable implant-supported denture (also an implant-supported overdenture[32]: 31 ) is a removable prosthesis which replaces teeth, using implants to improve support, retention and stability. They are most commonly complete dentures (as opposed to partial), used to restore edentulous dental arches.[25] The dental prosthesis can be disconnected from the implant abutments with finger pressure by the wearer. To enable this, the abutment is shaped as a small connector (a button, ball, bar or magnet) which can be connected to analogous adapters in the underside of the dental prosthesis.
Dental implants are used in orthodontic patients to replace missing teeth or as a temporary anchorage device (TAD) to facilitate orthodontic movement by providing an additional anchorage point.[31][33] For teeth to move, a force must be applied to them in the direction of the desired movement. The force stimulates cells in the periodontal ligament to cause bone remodeling, removing bone in the direction of travel of the tooth and adding it to the space created. In order to generate a force on a tooth, an anchor point (something that will not move) is needed. Since implants do not have a periodontal ligament, and bone remodelling will not be stimulated when tension is applied, they are ideal anchor points in orthodontics. Typically, implants designed for orthodontic movement are small and do not fully osseointegrate, allowing easy removal following treatment.[34] They are indicated when needing to shorten treatment time, or as an alternative to extra-oral anchorage. Mini-implants are frequently placed between the roots of teeth, but may also be sited in the roof of the mouth. They are then connected to a fixed brace to help move the teeth.
The introduction of small-diameter implants has provided dentists the means of providing edentulous and partially edentulous patients with immediate functioning transitional prostheses while definitive restorations are being fabricated. Many clinical studies have been done on the success of long-term usage of these implants. Based on the findings of many studies, mini dental implants exhibit excellent survival rates in the short to medium term (3–5 years). They appear to be a reasonable alternative treatment modality to retain mandibular complete overdentures from the available evidence.[35][36]
A typical conventional implant consists of a titanium screw (resembling a tooth root) with a roughened or smooth surface. The majority of dental implants are made of commercially pure titanium, which is available in four grades depending upon the amount of carbon, nitrogen, oxygen and iron contained.[37] Cold work hardened CP4 (maximum impurity limits of N .05 percent, C .10 percent, H .015 percent, Fe .50 percent, and O .40 percent) is the most commonly used titanium for implants. Grade 5 titanium, Titanium 6AL-4V (signifying the titanium alloy containing 6 percent aluminium and 4 percent vanadium alloy) is slightly harder than CP4 and used in the industry mostly for abutment screws and abutments.[38]: 284–285 Most modern dental implants also have a textured surface (through etching, anodic oxidation or various-media blasting) to increase the surface area and osseointegration potential of the implant.[39]: 55 If C.P. titanium or a titanium alloy has more than 85% titanium content, it will form a titanium-biocompatible titanium oxide surface layer or veneer that encloses the other metals, preventing them from contacting the bone.[40]
Ceramic (zirconia-based) implants exist in one-piece (combining the screw and the abutment) or two-piece systems – the abutment being either cemented or screwed – and might lower the risk for peri‐implant diseases, but long-term data on success rates is missing.[41]
Planning for dental implants focuses on the general health condition of the patient, the local health condition of the mucous membranes and the jaws and the shape, size, and position of the bones of the jaws, adjacent and opposing teeth. There are few health conditions that absolutely preclude placing implants[example needed] and there are certain conditions that can increase the risk of failure. Those with poor oral hygiene, heavy smokers and diabetics are all at greater risk for a variant of gum disease that affects implants called peri-implantitis, increasing the chance of long-term failures. Long-term steroid use, osteoporosis and other diseases that affect the bones can increase the risk of early failure of implants.[30]: 199 It has been suggested that radiotherapy can negatively affect the survival of implants.[11][42] Nevertheless, a systemic study published in 2016 concluded that dental implants installed in the irradiated area of an oral cavity may have a high survival rate, provided that the patient maintains oral hygiene measures and regular follow-ups to prevent complications.[43]
The long-term success of implants is determined in part by the forces they have to support. As implants have no periodontal ligament, there is no sensation of pressure when biting so the forces created are higher. To offset this, the location of implants must distribute forces evenly across the prosthetics they support.[44]: 15–39 Concentrated forces can result in fracture of the bridgework, implant components, or loss of bone adjacent the implant.[45] The ultimate location of implants is based on both biologic (bone type, vital structures, health) and mechanical factors. Implants placed in thicker, stronger bone like that found in the front part of the bottom jaw have lower failure rates than implants placed in lower density bone, such as the back part of the upper jaw. People who grind their teeth also increase the force on implants and increase the likelihood of failures.[30]: 201–208 [46][47][48][49]
The design of implants has to account for a lifetime of real-world use in a person's mouth. Regulators and the dental implant industry have created a series of tests to determine the long-term mechanical reliability of implants in a person's mouth where the implant is struck repeatedly with increasing forces (similar in magnitude to biting) until it fails.[50] When a more exacting plan is needed beyond clinical judgment, the dentist will make an acrylic guide (called a stent) prior to surgery which guides optimal positioning of the implant. Increasingly, dentists opt to get a CT scan of the jaws and any existing dentures, then plan the surgery on CAD/CAM software. The stent can then be made using stereolithography following computerized planning of a case from the CT scan. The use of CT scanning in complex cases also helps the surgeon identify and avoid vital structures such as the inferior alveolar nerve and the sinus.[51][52]: 1199
The use of bone-building drugs, like bisphosphonates and anti-RANKL drugs, requires special consideration with implants because they have been associated with a disorder called medication-associated osteonecrosis of the jaw (MRONJ). The drugs change bone turnover, which is thought to put people at risk for death of bone when having minor oral surgery. At routine doses (for example, those used to treat routine osteoporosis) the effects of the drugs linger for months or years but the risk appears to be very low. Because of this duality, uncertainty exists in the dental community about how to best manage the risk of BRONJ when placing implants. A 2009 position paper by the American Association of Oral and Maxillofacial Surgeons discussed that the risk of BRONJ from low dose oral therapy (or slow-release injectable) as between 0.01 and 0.06 percent for any procedure done on the jaws (implant, extraction, etc.). The risk is higher with intravenous therapy, procedures on the lower jaw, people with other medical issues, those on steroids, those on more potent bisphosphonates and people who have taken the drug for more than three years. The position paper recommends against placing implants in people who are taking high-dose or high-frequency intravenous therapy for cancer care. Otherwise, implants can generally be placed[53] and the use of bisphosphonates does not appear to affect implant survival.[54] Additional precaution can be taken by administering pentoxifylline and tocopherol both pre-operatively and post-operatively.[55] Moreover, patients taking bisphosphonates present a higher risk of implant failure in comparison to patients not taking this class of drugs.[7][8]
Most implant systems have five basic steps for placement of each implant:[30]: 214–221
There are different approaches to placement dental implants after tooth extraction.[57] The approaches are:
An increasingly common strategy to preserve bone and reduce treatment times includes the placement of a dental implant into a recent extraction site. On the one hand, it shortens treatment time and can improve aesthetics because the soft tissue envelope is preserved. On the other hand, implants may have a slightly higher rate of initial failure. Conclusions on this topic are difficult to draw, however, because few studies have compared immediate and delayed implants in a scientifically rigorous manner.[57]
After an implant is placed the internal components are covered with either a healing abutment, or a cover screw. A healing abutment passes through the mucosa, and the surrounding mucosa is adapted around it. A cover screw is flush with the surface of the dental implant, and is designed to be completely covered by mucosa. After an integration period, a second surgery is required to reflect the mucosa and place a healing abutment.[58]: 190–1
In the early stages of implant development (1970−1990) implant systems used a two-stage approach, believing that it improved the odds of initial implant survival. Subsequent research suggests that no difference in implant survival existed between one-stage and two-stage surgeries, and the choice of whether or not to "bury" the implant in the first stage of surgery became a concern of soft tissue (gingiva) management.[59] When tissue is inadequate, deficient or mutilated by the loss of teeth, adjacent bone or gingiva, implants are placed and allowed to osseointegrate, then the gingival flat is surgically placed around the healing abutments. The downside of a two-stage technique is the need for additional surgery and compromise of circulation to the tissue due to repeated surgeries.[60]: 9–12 The choice of one or two stages now centers around how best to reconstruct the soft tissues around lost teeth.
For an implant to osseointegrate, it needs to be surrounded by a healthy quantity of bone. In order for it to survive long-term, it needs to have a thick healthy soft tissue (gingiva) envelope around it. It is common for either the bone or soft tissue to be so deficient that the surgeon needs to reconstruct it either before or during implant placement.[52]: 1084 All techniques of augmenting the alveolar bone in preparation for implant placement are invasive and associated with a degree of morbidity.[61]
Bone grafting is necessary when there is a lack of bone. It also helps to stabilize the implant by increasing survival rates of the implant and decreasing marginal bone level loss.[62] While there are always new implant types, such as short implants, and techniques to allow compromise, a general treatment goal is to have a minimum of 10 mm (0.39 in) in bone height, and 6 mm (0.24 in) in width. Alternatively, bone defects are graded from A to D (A=10+ mm of bone, B=7–9 mm, C=4–6 mm and D=0–3 mm) where an implant's likelihood of osseointegrating is related to the grade of bone.[63]: 250
To achieve an adequate width and height of bone, various bone grafting techniques have been developed. The most frequently used is called guided bone graft augmentation where a defect is filled with either natural (harvested or autograft) bone or allograft (donor bone or synthetic bone substitute), covered with a semi-permeable membrane and allowed to heal. During the healing phase, natural bone replaces the graft, forming a new bony base for the implant.[58]: 223
Three common procedures are:[63]: 236
Other, more invasive procedures, also exist for larger bone defects including mobilization of the inferior alveolar nerve to allow placement of a fixture, onlay bone grafting using the iliac crest or another large source of bone and microvascular bone graft where the blood supply to the bone is transplanted with the source bone and reconnected to the local blood supply.[44]: 5–6 The final decision about which bone grafting technique that is best is based on an assessment of the degree of vertical and horizontal bone loss that exists, each of which is classified into mild (2–3 mm loss), moderate (4–6 mm loss) or severe (greater than 6 mm loss).[64]: 17 Orthodontic extrusion or orthodontic implant site development can be used in selected cases for vertical/horizontal alveolar augmentation.[65]
The gingiva surrounding a tooth has a 2–3 mm band of bright pink, very strong attached mucosa, then a darker, larger area of unattached mucosa that folds into the cheeks. When replacing a tooth with an implant, a band of strong, attached gingiva is needed to keep the implant healthy in the long-term. This is especially important with implants because the blood supply is more precarious in the gingiva surrounding an implant, and is theoretically more susceptible to injury because of a longer attachment to the implant than on a tooth (a longer biologic width).[66]: 629–633
When an adequate band of attached tissue is absent, it can be recreated with a soft tissue graft. There are four methods that can be used to transplant soft tissue. A roll of tissue adjacent to an implant (referred to as a palatal roll) can be moved towards the lip (buccal), gingiva from the palate can be transplanted, deeper connective tissue from the palate can be transplanted or, when a larger piece of tissue is needed, a finger of tissue based on a blood vessel in the palate (called a vascularized interpositional periosteal-connective tissue (VIP-CT) flap) can be repositioned to the area.[60]: 113–188 Xenogeneic collagen matrices are used for gingival augmentation after dental implantation.[67][68]
Additionally, for an implant to look esthetic, a band of full, plump gingiva is needed to fill in the space on either side of implant. The most common soft tissue complication is called a black triangle, where the papilla (the small triangular piece of tissue between two teeth) shrinks back and leaves a triangular void between the implant and the adjacent teeth. Dentists can only expect 2–4 mm of papilla height over the underlying bone. A black triangle can be expected if the distance between where the teeth touch and bone is any greater.[52]: 81–84
Alveolar bone resorption is a common side effect of tooth removal (extraction) due to severe tooth decay, trauma, or infection that limits dental implant placement. Surgical bone augmentation is associated with limitations such as high cost, bone graft rejection or failure, pain, infection, and the addition of 6–12 months to the treatment time till the graft matures. Compared with invasive bone augmentation surgery, orthodontic tooth movement has the capacity to regenerate the deficient alveolar ridge and create adequate bone volume for implant placement. This is particularly useful when restoring one or two missing teeth with implants; however, the orthodontic implant site-switching technique[69][70] can only be used when there is an edentulous area adjacent to healthy teeth that can be moved orthodontically into the edentulous site and generate healthy bone volume for implant placement.[71]
Orthodontic tooth movement can generate new bone.[72] This is because of the fibres of the periodontal ligament (PDL) surrounding the teeth and attached to the alveolar bone, the stretched fibres in the PDL stimulate the osteoblasts depositing new alveolar bone. For instance, the orthodontic forced eruption of hopeless teeth can augment the bone vertically and eliminate or reduce the amount of bone graft required prior to implant placement.[73] Similarly, where there is a bone-deficient edentulous (toothless) site, it is possible to move the healthy adjacent teeth into this area, closing the edentulous space and simultaneously creating an implant site with enough bone adjacent to where implant placement was originally planned.[74][75][76]

The prosthetic phase begins once the implant is well integrated (or has a reasonable assurance that it will integrate) and an abutment is in place to bring it through the mucosa. Even in the event of early loading (less than three months), many practitioners will place temporary teeth until osseointegration is confirmed. The prosthetic phase of restoring an implant requires an equal amount of technical expertise as the surgical because of the biomechanical considerations, especially when multiple teeth are to be restored. The dentist will work to restore the vertical dimension of occlusion, the esthetics of the smile, and the structural integrity of the teeth to evenly distribute the forces of the implants.[30]: 241–251
There are various options for when to attach teeth to dental implants,[77] classified into:
For an implant to become permanently stable, the body must grow bone to the surface of the implant (osseointegration). Based on this biologic process, it was thought that loading an implant during the osseointegration period would result in movement that would prevent osseointegration, and thus increase implant failure rates. As a result, three to six months of integrating time (depending on various factors) was allowed before placing the teeth on implants (restoring them).[30] However, later research suggests that the initial stability of the implant in bone is a more important determinant of success of implant integration, rather than a certain period of healing time. As a result, the time allowed to heal is typically based on the density of bone the implant is placed in and the number of implants splinted together, rather than a uniform amount of time. When implants can withstand high torque (35 Ncm) and are splinted to other implants, there are no meaningful differences in long-term implant survival or bone loss between implants loaded immediately, at three months, or at six months.[77] The corollary is that single implants, even in solid bone, require a period of no-load to minimize the risk of initial failure.[78]
An abutment is selected depending on the application. In many single crown and fixed partial denture scenarios (bridgework), custom abutments are used. An impression of the top of the implant is made with the adjacent teeth and gingiva. A dental lab then simultaneously fabricates an abutment and crown. The abutment is seated on the implant, a screw passes through the abutment to secure it to an internal thread on the implant (lag-screw). There are variations on this, such as when the abutment and implant body are one piece or when a stock (prefabricated) abutment is used. Custom abutments can be made by hand, as a cast metal piece or custom milled from metal or zirconia, all of which have similar success rates.[52]: 1233
The platform between the implant and the abutment can be flat (buttress) or conical fit. In conical fit abutments, the collar of the abutment sits inside the implant which allows a stronger junction between implant and abutment and a better seal against bacteria into the implant body. To improve the gingival seal around the abutment collar, a narrowed collar on the abutment is used, referred to as platform switching. The combination of conical fits and platform switching gives marginally better long term periodontal conditions compared to flat-top abutments.[79][80]
Regardless of the abutment material or technique, an impression of the abutment is then taken and a crown secured to the abutment with dental cement. Another variation on abutment/crown model is when the crown and abutment are one piece and the lag-screw traverses both to secure the one-piece structure to the internal thread on the implant. There does not appear to be any benefit, in terms of success, for cement versus screw-retained prosthetics, although the latter is believed to be easier to maintain (and change when the prosthetic fractures) and the former offers high esthetic performance.[52]: 1233
When a removable denture is worn, retainers to hold the denture in place can be either custom made or "off-the-shelf" (stock) abutments. When custom retainers are used, four or more implant fixtures are placed and an impression of the implants is taken and a dental lab creates a custom metal bar with attachments to hold the denture in place. Significant retention can be created with multiple attachments and the use of semi-precision attachments (such as a small diameter pin that pushes through the denture and into the bar) which allows for little or no movement in the denture, but it remains removable.[32]: 33–34 However, the same four implants angled in such a way to distribute occlusal forces may be able to safely hold a fixed denture in place with comparable costs and number of procedures giving the denture wearer a fixed solution.[81]
Alternatively, stock abutments are used to retain dentures using a male-adapter attached to the implant and a female adapter in the denture. Two common types of adapters are the ball-and-socket style retainer and the button-style adapter. These types of stock abutments allow movement of the denture, but enough retention to improve the quality of life for denture wearers, compared to conventional dentures.[82] Regardless of the type of adapter, the female portion of the adapter that is housed in the denture will require periodic replacement, however the number and adapter type does not seem to affect patient satisfaction with the prosthetic for various removable alternatives.[83]
After placement, implants need to be cleaned (similar to natural teeth) with a periodontal scaler to remove any plaque. Because of the more precarious blood supply to the gingiva, care should be taken with dental floss. Implants will lose bone at a rate similar to natural teeth in the mouth (e.g. if someone has periodontal disease, an implant can be affected by a similar disorder) but will otherwise last. The porcelain on crowns should be expected to discolour, fracture or require repair approximately every ten years, although there is significant variation in the service life of dental crowns based on the position in the mouth, the forces being applied from opposing teeth and the restoration material. Where implants are used to retain a complete denture, depending on the type of attachment, connections need to be changed or refreshed every one to two years.[44]: 76 An oral irrigator may also be useful for cleaning around implants.[84]
The same kinds of techniques used for cleaning teeth are recommended for maintaining hygiene around implants, and can be manually or professionally administered.[85] Examples of this would be using soft toothbrushes or nylon-coated interproximal brushes.[85] The one implication during professional treatment is that metal instruments may cause damage to the metallic surface of the implant or abutment, which can lead to bacterial colonisation.[85] To avoid this, there are specially designed instruments made with hard plastic or rubber. Additionally rinsing (twice daily) with antimicrobial mouthwashes has been shown to be beneficial.[85] There is no evidence that one type of antimicrobial is better than the other.[85]
Peri-implantitis is a condition that may occur with implants due to bacteria, plaque, or design and it is on the rise.[85][86][87] This disease begins as a reversible condition called peri-implant mucositis but can progress to peri-implantitis if left untreated, which can lead to implant failure.[86][85] People are encouraged to discuss oral hygiene and maintenance of implants with their dentists.[85][86][87] There are different interventions if peri-implantitis occurs, such as mechanical debridement, antimicrobial irrigation, and antibiotics. There can also be surgery such as open-flap debridement to remove bacteria, assess/smooth implant surface, or decontaminate implant surface.[86] There is not enough evidence to know which intervention is best in the case of peri-implantitis.[86]
Placement of dental implants is a surgical procedure and carries the normal risks of surgery including infection, excessive bleeding and necrosis of the flap of tissue around the implant. Nearby anatomic structures, such as the inferior alveolar nerve, the maxillary sinus and blood vessels, can also be injured when the osteotomy is created or the implant placed.[88][89] Even when the lining of the maxillary sinus is perforated by an implant, long term sinusitis is rare.[90][91] An inability to place the implant in bone to provide stability of the implant (referred to as primary stability of the implant) increases the risk of failure to osseointegration.[44]: 68
Primary implant stability refers to the stability of a dental implant immediately after implantation. The stability of the titanium screw implant in the patient's bone tissue post surgery may be non-invasively assessed using resonance frequency analysis. Sufficient initial stability may allow immediate loading with prosthetic reconstruction, though early loading poses a higher risk of implant failure than conventional loading.[92]
The relevance of primary implant stability decreases gradually with regrowth of bone tissue around the implant in the first weeks after surgery, leading to secondary stability. Secondary stability is different from the initial stabilization, because it results from the ongoing process of bone regrowth into the implant (osseointegration). When this healing process is complete, the initial mechanical stability becomes biological stability. Primary stability is critical to implantation success until bone regrowth maximizes mechanical and biological support of the implant. Regrowth usually occurs during the 3–4 weeks after implantation. Insufficient primary stability, or high initial implant mobility, can lead to failure.
An implant is tested between 8 and 24 weeks to determine if it is integrated. There is significant variation in the criteria used to determine implant success, the most commonly cited criteria at the implant level are the absence of pain, mobility, infection, gingival bleeding, radiographic lucency or peri-implant bone loss greater than 1.5 mm.[94] Dental implant success is related to operator skill,[95] quality and quantity of the bone available at the site,[4] and the patient's oral hygiene, but the most important factor is primary implant stability.[96] While there is significant variation in the rate that implants fail to integrate (due to individual risk factors), the approximate values are 1 to 6 percent[44]: 68 [77] Integration failure is rare, particularly if a dentist's or oral surgeon's instructions are followed closely by the patient. Immediate loading implants may have a higher rate of failure, potentially due to being loaded immediately after trauma or extraction, but the difference with proper care and maintenance is well within statistical variance for this type of procedure. More often, osseointegration failure occurs when a patient is either too unhealthy to receive the implant or engages in behavior that contraindicates proper dental hygiene including smoking[97][98][99] or drug use.
The long-term complications that result from restoring teeth with implants relate directly to the risk factors of the patient and the technology. There are the risks associated with appearance including a high smile line, poor gingival quality and missing papillae, difficulty in matching the form of natural teeth that may have unequal points of contact or uncommon shapes, bone that is missing, atrophied or otherwise shaped in an unsuitable manner, unrealistic expectations of the patient or poor oral hygiene. The risks can be related to biomechanical factors, where the geometry of the implants does not support the teeth in the same way the natural teeth did such as when there are cantilevered extensions, fewer implants than roots or teeth that are longer than the implants that support them (a poor crown-to-root ratio). Similarly, grinding of the teeth, lack of bone or low diameter implants increase the biomechanical risk.[100] : 27–51 Finally there are technological risks, where the implants themselves can fail due to fracture or a loss of retention to the teeth they are intended to support.[100]: 27–51
Beyond the possibility of mechanical failure[101] which may be due to poor prosthetic fitment, wear and tear, or user-induced actions such as bruxism, dental implants are also subject to peri-implant mucositis and peri-implantitis, where gum tissue and bone mass around the implant are resorbed, and the implant gradually becomes loose, and has to be removed.[102][103] In addition, although titanium is generally well tolerated by the body, there have been cases where the build-up of titanium particles released by the implant may cause systemic inflammatory response.[104] Because there is no dental enamel on an implant, it does not fail due to cavities like natural teeth. While large-scale, long-term studies are scarce, several systematic reviews estimate the long-term (five to ten years) survival of dental implants at 93–98 percent depending on their clinical use.[17][18][19] During initial development of implant retained teeth, all crowns were attached to the teeth with screws, but more recent advancements have allowed placement of crowns on the abutments with dental cement (akin to placing a crown on a tooth). This has created the potential for cement, that escapes from under the crown during cementation to get caught in the gingiva and create a peri-implantitis (see picture below). While the complication can occur, there does not appear to be any additional peri-implantitis in cement-retained crowns compared to screw-retained crowns overall.[105]
In compound implants (two stage implants), between the actual implant and the superstructure (abutment) are gaps and cavities into which bacteria can penetrate from the oral cavity. Later these bacteria will return into the adjacent tissue and can cause periimplantitis. Criteria for the success of the implant supported dental prosthetic varies from study to study, but can be broadly classified into failures due to the implant, soft tissues or prosthetic components or a lack of satisfaction on the part of the patient. The most commonly cited criteria for success are function of at least five years in the absence of pain, mobility, radiographic lucency and peri-implant bone loss of greater than 1.5 mm on the implant, the lack of suppuration or bleeding in the soft tissues and occurrence of technical complications/prosthetic maintenance, adequate function, and esthetics in the prosthetic. In addition, the patient should ideally be free of pain, paraesthesia, able to chew and taste and be pleased with the esthetics.[94]
The rates of complications vary by implant use and prosthetic type and are listed below:
The most common complication being fracture or wear of the tooth structure, especially beyond ten years[19][20] with fixed dental prostheses made of metal-ceramic having significantly higher ten-year survival compared those made of gold-acrylic.[19]




There is archeological evidence that humans have attempted to replace missing teeth with root form implants for thousands of years. Remains from ancient China (dating 4000 years ago) have carved bamboo pegs, tapped into the bone, to replace lost teeth, and 2000-year-old remains from ancient Egypt have similarly shaped pegs made of precious metals. Some Egyptian mummies were found to have transplanted human teeth, and in other instances, teeth made of ivory.[23]: 26 [109][110] Etruscans produced the first pontics using single gold bands as early as 630 BC and perhaps earlier.[111][112] Wilson Popenoe and his wife in 1931, at a site in Honduras dating back to 600 AD, found the lower mandible of a young Mayan woman, with three missing incisors replaced by pieces of sea shells, shaped to resemble teeth.[113] Bone growth around two of the implants, and the formation of calculus, indicates that they were functional as well as esthetic. The fragment is currently part of the Osteological Collection of the Peabody Museum of Archaeology and Ethnology at Harvard University.[23][109]
In modern times, a tooth replica implant was reported as early as 1969, but the polymethacrylate tooth analogue was encapsulated by soft tissue rather than osseointegrated.[114]
The early part of the 20th century saw a number of implants made of a variety of materials. One of the earliest successful implants was the Greenfield implant system of 1913 (also known as the Greenfield crib or basket).[115] Greenfield's implant, an iridioplatinum implant attached to a gold crown, showed evidence of osseointegration and lasted for a number of years.[115] The first use of titanium as an implantable material was by Bothe, Beaton and Davenport in 1940, who observed how close the bone grew to titanium screws, and the difficulty they had in extracting them.[116] Bothe et al. were the first researchers to describe what would later be called osseointegration (a name that would be marketed later on by Per-Ingvar Brånemark). In 1951, Gottlieb Leventhal implanted titanium rods in rabbits.[117] Leventhal's positive results led him to believe that titanium represented the ideal metal for surgery.[117]
In the 1950s research was being conducted at Cambridge University in England on blood flow in living organisms. These workers devised a method of constructing a chamber of titanium which was then embedded into the soft tissue of the ears of rabbits. In 1952 the Swedish orthopaedic surgeon, Per-Ingvar Brånemark, was interested in studying bone healing and regeneration. During his research time at Lund University he adopted the Cambridge designed "rabbit ear chamber" for use in the rabbit femur. Following the study, he attempted to retrieve these expensive chambers from the rabbits and found that he was unable to remove them. Brånemark observed that bone had grown into such close proximity with the titanium that it effectively adhered to the metal. Brånemark carried out further studies into this phenomenon, using both animal and human subjects, which all confirmed this unique property of titanium.[118] Leonard Linkow, in the 1950s, was one of the first to insert titanium and other metal implants into the bones of the jaw. Artificial teeth were then attached to these pieces of metal.[119] In 1965 Brånemark placed his first titanium dental implant into a human volunteer. He began working in the mouth as it was more accessible for continued observations and there was a high rate of missing teeth in the general population offered more subjects for widespread study. He termed the clinically observed adherence of bone with titanium as "osseointegration".[66]: 626 Since then implants have evolved into three basic types:
Tooth whitening or tooth bleaching is the process of lightening the colour of human teeth.[1] Whitening is often desirable when teeth become yellowed over time for a number of reasons, and can be achieved by changing the intrinsic or extrinsic colour of the tooth enamel.[2] The chemical degradation of the chromogens within or on the tooth is termed as bleaching.[1]
Hydrogen peroxide (H
2O
2) is the active ingredient most commonly used in whitening products and is delivered as either hydrogen peroxide or carbamide peroxide.[1] Hydrogen peroxide is analogous to carbamide peroxide as it is released when the stable complex is in contact with water. When it diffuses into the tooth, hydrogen peroxide acts as an oxidising agent that breaks down to produce unstable free radicals. In the spaces between the inorganic salts in tooth enamel, these unstable free radicals attach to organic pigment molecules resulting in small, less heavily pigmented components.[3] Reflecting less light, these smaller molecules create a "whitening effect".[3] Peroxyacids are an alternative to hydrogen peroxide and also contribute to the breakdown of pigment molecules. There are different products available on the market to remove stains.[1] For whitening treatment to be successful, dental professionals (dental hygienist or dentist) should correctly diagnose the type, intensity and location of the tooth discolouration.[3] Time exposure and the concentration of the bleaching compound determines the tooth whitening endpoint.[1]
The perception of tooth colour is multi-factorial. Reflection and absorption of light by the tooth can be influenced by a number of factors, including specular transmission of light through the tooth, specular reflection at the surface, diffuse light reflection at the surface, absorption and scattering of light within the dental tissues, enamel mineral content, enamel thickness, dentine colour, the human observer, the fatigue of the eye, the type of incident light, and the presence of extrinsic and intrinsic stains.[4] Additionally, the perceived brightness of the tooth can change depending on the brightness and colour of the background.[4]
The combination of intrinsic colour and the presence of extrinsic stains on the tooth surface influence the colour and thus the overall appearance of teeth.[2] The scattering of light and absorption within enamel and dentine determine the intrinsic colour of teeth and because the enamel is relatively translucent, the dentinal properties can play a major role in determining the overall tooth colour.[4] On the other hand, extrinsic stain and colour is the result of coloured regions that have formed within the acquired pellicle on the enamel surface and can be influenced by lifestyle behaviours or habits.[2] For example, dietary intake of tannin-rich foods, poor tooth brushing technique, tobacco products, and exposure to iron salts and chlorhexidine can darken the colour of a tooth.[2]
With increasing age, teeth tend to grow darker in shade.[5] This can be attributed to secondary dentin formation and thinning of enamel due to tooth wear which contributes to a significant decrease in lightness and increase in yellowness.[5] Tooth shade is not influenced by gender or race.[5]
Tooth discolouration and staining is primarily due to two sources of stain: intrinsic and extrinsic (see Figure 2).[1] In essence, tooth whitening primarily targets those intrinsic stains in which cannot be removed through mechanics such as a debridement (clean) or prophylaxis, in the dental office.[6] Below explains in-depth the differences between the two sources of which contribute to such discolouration of the tooth's surface.

Extrinsic staining, is largely due to environmental factors including smoking, pigments in beverages and foods, antibiotics, and metals such as iron or copper. Coloured compounds from these sources are adsorbed into acquired dental pellicle or directly onto the surface of the tooth causing a stain to appear.[7]
Extrinsic staining may be removed through various treatment methods:
Intrinsic staining primarily occurs during the tooth development either before birth or at early childhood. Intrinsic stains are those that cannot be removed through mechanical measures such as debridement or a prophylactic stain removal. As the age of the person increases, the teeth can also appear yellower over time.[15] Below are examples of intrinsic sources of stains:
Prior to proceeding to tooth whitening alternatives, it is advised that the patient comes into the dental office to have a comprehensive oral examination that consists of a full medical, dental, and social history. This will allow the clinician to see if there is any treatment that needs to be done such as restorations to remove cavities, and to assess whether or not the patient will be a good candidate to have the whitening done. The clinician would then debride (clean) the tooth surface with an ultrasonic scaler, hand instruments, and potentially a prophy paste to remove extrinsic stains as mentioned above. This will allow a clean surface for maximum benefits of whichever tooth whitening method the patient chooses.[6] Below will discuss the various types of tooth whitening methods including both internal application of bleaching and external application through the use of bleaching agents.
Before the treatment, the clinician should examine the patient: taking a health and dental history (including allergies and sensitivities), observe hard and soft tissues, placement and conditions of restorations, and sometimes x-rays to determine the nature and depth of possible irregularities. If this is not completed prior to the whitening agents being applied to the tooth surface, excessive sensitivity and other complications may occur.

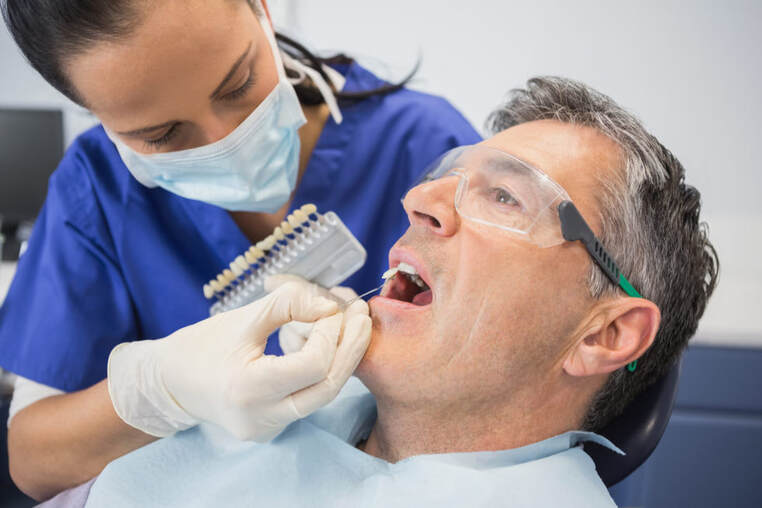
The whitening shade guides are used to measure tooth colour. These shades determine the effectiveness of the whitening procedure, which may vary from two to seven shades.[34] These shades may be reached after a single in office appointment, or may take longer, depending on the individual. The effects of bleaching can last for several months, but may vary depending on the lifestyle of the patient. Consuming tooth staining foods or drinks that have a strong colour may compromise effectiveness of the treatment. These include food and drinks containing tannins such as; coffee, tea, red wines, and curry.
In-office bleaching procedures generally use a light-cured protective layer that is carefully painted on the gums and papilla (the tips of the gums between the teeth) to reduce the risk of chemical burns to the soft tissues. The bleaching agent is either carbamide peroxide, which breaks down in the mouth to form hydrogen peroxide, or hydrogen peroxide itself. The bleaching gel typically contains between 10% and 44% carbamide peroxide, which is roughly equivalent to a 3% to 16% hydrogen peroxide concentration. The legal percentage of hydrogen peroxide allowed to be given is 0.1–6%.[where?] Bleaching agents are only allowed to be given by dental practitioners, dental therapists, and dental hygienists.
Bleaching is least effective when the original tooth color is grayish and may require custom bleaching trays. Bleaching is most effective with yellow discolored teeth. If heavy staining or tetracycline damage is present on a patient's teeth, and whitening is ineffective (tetracycline staining may require prolonged bleaching, as it takes longer for the bleach to reach the dentine layer), there are other methods of masking the stain. Bonding, which also masks tooth stains, is when a thin coating of composite material is applied to the front of a person's teeth and then cured with a blue light. A veneer can also mask tooth discoloration.
In-chair whitening is faster and more effective in comparison to the take-home bleaching options.[medical citation needed] Some clinicians also make custom bleaching trays, which can take up to a week to create. After the whitening treatment is completed, the patient is able to use these trays for maintenance of their bleaching with at-home kits or for use with desensitising products.
Power or light-accelerated bleaching uses light energy which is intended to accelerate the process of bleaching in a dental office. Different types of energy can be used in this procedure, with the most common being halogen, LED, or plasma arc. Use of light during bleaching increases the risk of tooth sensitivity and may not be any more effective than bleaching without light when high concentrations of hydrogen peroxide are used.[35] A 2015 study showed that the use of a light activator does not improve bleaching, has no measurable effect, and rather is likely to increase the temperature of the associated tissues, resulting in damage.[36][37]
The ideal source of energy should be high energy to excite the peroxide molecules without overheating the pulp of the tooth.[38] Lights are typically within the blue light spectrum as this has been found to contain the most effective wavelengths for initiating the hydrogen peroxide reaction. A power bleaching treatment typically involves isolation of soft tissue with a resin-based, light-curable barrier, application of a professional dental-grade hydrogen peroxide whitening gel (25–38% hydrogen peroxide), and exposure to the light source for 6–15 minutes. Recent technical advances have minimized heat and UV emissions, allowing for a shorter patient preparation procedure.
For any whitening treatments, it is recommended that a comprehensive examination of the patient is done including the use of radiographs to aid in the diagnosis of the current condition of the mouth, including any allergies that may be present. The patient will need to have a healthy mouth and free of periodontal disease or cavities and to have had a debridement/clean done to remove any tartar or plaque build up.[39]
It is recommended to avoid smoking, drinking red wine, eating or drinking any deeply coloured foods after this as the teeth may stain considerably straight after treatment.
Internal bleaching is a process which occurs after a tooth has been endodontically treated. This means that the tooth will have had the nerve of the tooth extirpated or removed through a root canal treatment at the dentist or by a specialist endodontist. Internal bleaching is often sought after in teeth which have been endodontically treated as tooth discolouration becomes a problem due to the lack of nerve supply to that tooth. It is common to have this internal bleaching done on an anterior tooth (a front tooth that you can see when smiling and talking). A way around this is by sealing off the bleaching agent inside the tooth itself and replacing it every few weeks until the desired shade has been achieved. The amount of time between appointments varies from patient to patient and with operator preference until the desired shade has been achieved.[40] Even though this is a great option, the disadvantage of this treatment is a risk of internal root resorption of the tooth that is being internally bleached. This may not occur in every patient or every tooth, and its occurrence is difficult to determine prior to completing the treatment.[40]

At home tooth whitening products are available from dentists or 'over the counter' (OTC).[41] At home whitening methods include over-the-counter strips and gels, whitening rinses, whitening toothpastes, and tray-based tooth whiteners.[41] OTC products can be used for milder cases of tooth staining.[41] Home-based bleaching (following manufacturer's instructions) results in less tooth sensitivity than in-office bleaching.[42]
The plastic whitening strips contain a thin layer of peroxide gel and are shaped to fit the buccal/labial surfaces of teeth.[1] Many different types of whitening strips are available on the market, after being introduced in the late 1980s.[1] Specific whitening strip products have their own set of instructions however the strips are typically applied twice daily for 30 minutes for 14 days.[1] In several days, tooth colour can lighten by 1 or 2 shades.[1] The tooth whitening endpoint does depend on the frequency of use and ingredients of the product.[1]
Whitening gels are applied onto the tooth surface with a small brush.[1] The gels contain peroxide and are recommended to be applied twice a day for 14 days.[1] The tooth whitening endpoint like that of the whitening strips.[1]
Whitening rinses work by reaction of the oxygen sources such as hydrogen peroxide within the rinse and the chromogens on or within the tooth.[1] It is recommended to use twice a day, rinsing for one minute.[1] To see an improvement in shade colour, it can take up to three months.[1]
Whitening toothpastes differ from regular toothpastes in that they contain higher amounts of abrasives and detergents to be more effective at removing tougher stains.[1] Some whitening toothpastes contain low concentrations of carbamide peroxide or hydrogen peroxide which help lighten tooth colour however they do not contain bleach (sodium hypochlorite).[1] With continuity of use over time, tooth colour can lighten by one or two shades.[1]
Tray-based tooth whitening is achieved by wearing a fitted tray containing carbamide peroxide bleaching gel overnight or for two to four hours a day.[1] If manufacturer's instructions are followed, tooth whitening can occur within three days and lighten teeth by one or two shades.[1] This type of tooth whitening is available over-the-counter and professionally from an oral health professional.[1]
Baking soda is a safe, low abrasive, and effective stain removal and tooth whitening toothpaste.[43] Tooth whitening toothpaste that have excessive abrasivity are harmful to dental tissue, therefore baking soda is a desirable alternative.[43] To date, clinical studies on baking soda report that there have been no reported adverse effects.[43] It also contains acid-buffering components that makes baking soda biologically antibacterial at high concentrations and capable of preventing growth of Streptococcus mutans.[43] Baking soda might be useful for cavities-prone patients, as well as those who wish to have whiter teeth.[43]
Tooth whitening may be undertaken for a variety of reasons, but whitening may also be recommended to some individuals by dental professionals.[44]
Some groups are advised to carry out tooth whitening with caution as they may be at higher risk of adverse effects.
Some of the common side effects involved in teeth whitening are increased sensitivity of the teeth, gum irritation, and extrinsic teeth discolouration.[41]
The use of bleach with extremely low pH levels in the tooth whitening procedure may lead to hypersensitive teeth, as it causes the dentinal tubules to open.[47] Exposure to cold, hot, or sweet stimuli may further exacerbate the intensity of the hypersensitive response. Amongst those who receive in-office whitening treatment, between 67 and 78% of the individuals experience sensitivity after the procedure where hydrogen peroxide and heat is utilized.[48][49] Although it varies from person to person, sensitivity after whitening treatment can last up to 4–39 days.[50][51]
Potassium nitrate and sodium fluoride in toothpastes are used to ease discomfort following bleaching, however, there is no evidence to suggest that this is a permanent method to eradicate the issue of hypersensitivity.[52]
Hydrogen peroxide is an irritant and cytotoxic. Hydrogen peroxide with concentrations of 10% or higher can cause tissue damage, be corrosive to mucous membranes and cause burning sensation to the skin.[53] Chemical burns can commonly occur whilst bleaching, irritation and discolouration of the mucous membranes may occur if a high concentration of oxidising agent comes in to contact with unprotected tissue. Poorly fitting bleaching trays are amongst the most common reasons for chemical burns. The temporary burning induced by whitening treatments can be reduced by using custom-made plastic trays or nightguards provided by the dental professional. This prevents the leakage of solution onto the surrounding mucosa.[54]
Uneven results are quite common after bleaching. Consuming less foods and drinks that cause surface staining of teeth can contribute to attaining a good result from tooth whitening.
Nearly half the initial change in colour provided by an intensive in-office treatment (i.e., one hour treatment in a dentist's chair) may be lost in seven days.[55] Rebound is experienced when a large proportion of the tooth whitening has come from tooth dehydration (also a significant factor in causing sensitivity).[56] As the tooth rehydrates, tooth colour "rebounds", back toward where it started.[57]
Over-bleaching, more often known as the "bleached effect", occurs among treatments that promise a large change over a short period of time e.g., hours. Over-bleaching can emit a translucent and brittle appearance.[58]
Teeth enamel can have an adverse negative effect by whitening treatment.[59] Evidence from studies show that carbamide peroxide present in whitening gels can damage the enamel surface. Although this effect is not as damaging as phosphoric acid etch,[60] the increased irregularity of the teeth surface makes the teeth more susceptible to extrinsic staining, thus having an increased detrimental effect on the aesthetics. The increased porosity and changes in surface roughness may have an impact on the formation of supra- and subgingival plaque, thus increasing the adhesion of bacterial species such as Streptococcus mutans and Streptococcus sobrinus, significant contributors to dental cavities.[54] Dental restorations are susceptible to unacceptable colour change even when using the home-based systems.[1]
Intracoronal bleaching is a tooth whitening method that uses 30% more hydrogen peroxide. Such tooth whitening methods can weaken the mechanical properties of dentine and could potentially lead to severe tooth sensitivity.[61]
Dental restorations are susceptible to unacceptable colour change even when using the home-based systems.[1]
Ceramic crowns – aggressive bleaching can chemically react with ceramic crowns and reduce their stability.[1]
Dental amalgam – exposure to carbamide peroxide solutions increase mercury release for one to two days.[61][62] The release of amalgam components is said to be due to active oxidation. This increase in amalgam mercury release is proportional to the concentration of carbamide peroxide.[63]
Resin composite – bond strength between enamel and resin based fillings become weakened.[64] Many studies have found that 10–16% carbamide peroxide tooth bleaching gels (containing approximately 3.6–5.76% hydrogen peroxide) leads to an increase in the surface roughness and porosity of composite resins.[63] However, the saliva may exert a protective effect. In addition, changes in the reflectance of the composite have been analysed following whitening with high concentration (30–35%) hydrogen peroxide.[63] This suggests that tooth whitening negatively impacts composite resin restorations.[63]
Glass ionomer and other cements – studies suggest that solubility of these materials may increase.[65]
Bleachorexia is the term that is used to describe an individual that develops an unhealthy obsession with teeth whitening.[45] This condition is similar to body dysmorphic disorder. The characteristics of bleachorexia are the continuous use of whitening products even though the teeth cannot possibly become whiter, despite the provision of repeated treatment.[58] A person with bleachorexia will continually seek out for different whitening products, hence, it is recommended that a target shade is agreed upon before starting the treatment procedure to help with this problem.[58]
The use of personalised home whitening trays is a patient administered therapy that is prescribed and dispensed by a dentist.[66] Patients need to actively participate in their treatment and follow the guidelines given by the dentist accurately.[67] Erratic or inaccurate use of the bleaching trays could cause harm to the patient such as blistering or sensitivity of the teeth and the surrounding soft tissue.[68] Inconsistent use of the bleaching trays can lead to the slowing and irregularity of the whitening process.[69] Some patients with a substantial gag reflex may not be able to tolerate the trays and would need to consider other methods of teeth whitening.[67]
Hydrogen peroxide-based bleaching agents are always associated with Reactive Oxygen Species (ROS). The free radicals diffuse through the enamel and dentin and break down the color molecules, resulting in the perception of a whiter tooth color.[70] The downside is that these radicals have certain local harmful effects, such as enamel erosion, changes in the microhardness of the teeth, gum irritation, post-bleaching hypersensitivity, and burning sensations.[71] The following side effects are also known:
Bleaching agents based on peroxycarboxylic acids (PAP) can be chosen as an effective vehicle for tooth whitening. PAP has proven to be almost harmless to enamel with a safe and reliable bleaching effect.[74] In the clinical application of PAP for tooth whitening, oxidation reactions also occur, and color molecules are bleached through chemical-physical processes. However, the reaction occurs without the formation of free radicals. This is the major and decisive difference, as free radicals are the main cause of tooth sensitivity and gum irritation in tooth whitening with hydrogen peroxide-based bleaching agents.[75]
Evidence suggests that hydrogen peroxide might act as a tumour promoter.[76] Although cervical root resorption is more evidently observed in thermocatalytic bleaching methods, intracoronal internal bleaching may also lead to tooth root resorption.[76] Moreover, severe damage to intracoronal dentine and tooth crown fracture can occur due to this bleaching method.[76]
However, the International Agency of Research on Cancer (IARC) has concluded that there is insufficient evidence to prove that hydrogen peroxide is a carcinogen to humans.[77] Recently, the genotoxic potential of hydrogen peroxide was evaluated. The results indicated that the oral health products that contain or release hydrogen peroxide up to 3.6% will not increase the cancerous risk of an individual,[78] hence, it is safe to use in moderation.
Despite achieving the results of treatment, stains can return within an initial couple of months of treatment. Various methods may be employed to prolong the treatment results, such as:[citation needed]
Teeth whitening remedies have been present since ancient times. Despite seeming absurd, some methods were somewhat effective in their results.
Ancient Roman dentists believed in using urine with goat milk to make their teeth look whiter.[79][80][81] Pearly white teeth symbolized beauty and marked wealth. In the Auyrveda medicine system, oil pulling was used as an oral therapy. For this process today, swish coconut or olive oil in your mouth for up to 20 minutes each day. In the late 17th century, many people reached out to barbers, who used a file to file down the teeth before applying an acid that would, in fact, whiten the teeth. Although the procedure was successful, the teeth would become completely eroded and more prone to becoming decayed.[82] Guy de Chauliac suggested the following to whiten the teeth: "Clean the teeth gently with a mixture of honey and burnt salt to which some vinegar has been added."[83] In 1877, oxalic acid was proposed for whitening, followed by calcium hypochlorite.[83]
In the late 1920s, mouthwash containing pyrozone (ether peroxide) was found to reduce cavities while providing a whiter appearance to the teeth.[84] By 1940s and 1950s, ether and hydrogen peroxide gels were used to whiten vital teeth, whereas non-vital teeth were whitened using pyrozone and sodium perborate.[84]
In the late 1960s, Dr William Klusmeier, an Orthodontist from Fort Smith, Arkansas, introduced the custom tray bleaching. However, it was not until 1989 that Haywood and Heymann published an article in support of this method. Carbamide peroxide with a shelf life of one to two years, as opposed to hydrogen peroxide with a shelf life one to two months, was seen as a more stable agent for whitening teeth.[84]
Teeth whitening has become the most promoted and mentioned methodology in cosmetic dentistry. In excess of 100 million Americans brighten their teeth using different methods; spending $15 billion in 2010.[85] The US Food and Drug Administration only endorses gels that are under 6% hydrogen peroxide or 16% or less of carbamide peroxide. The Scientific Committee on Consumer Safety of the EU consider gels containing higher fixations can be dangerous.[citation needed]
As per European Council guidelines, only a certified dental professional can lawfully give tooth whitening products utilizing 0.1–6% hydrogen peroxide, provided the patient is 18 years of age or older.[86] In 2010, the UK General Dental Council became concerned of the "risk to patient safety from poor quality tooth whitening being carried out by untrained or poorly trained staff."[87] A public attitudes survey, conducted by the GDC, showed that 83% of people support "policies of regulating tooth whitening to protect patient safety and prosecuting illegal practice."[87] A group of dental professionals and associations called The Tooth Whitening Information Group (TWIG) was founded to advance protected and beneficial tooth whitening information and assistance to the general population. Reports can be made to the TWIG through their website with respect to any individual giving unlawful tooth whitening services, or if an individual has personally undergone treatment done by a non-dental professional.
In Brazil, all whitening items are classed as cosmetics (Degree II).[45] There are worries that this will increase abuse of whitening products and thus there have been calls for reanalysis.[45]
According to research, tooth whitening can produce positive changes in young participants' Oral Health Related Quality of Life (OHRQoL) in aesthetic areas such as smiling, laughing, and showing teeth without embarrassment. However, its main side-effect, tooth sensitivity, negatively affects quality of life.[88]
cite book: CS1 maint: publisher location (link)cite journal: CS1 maint: numeric names: authors list (link)The in-office bleaching treatment of vital teeth did not show improvement with the use of light activator sources for the purpose of accelerating the process of the bleaching gel and achieving better results.
citation: CS1 maint: DOI inactive as of July 2025 (link) CS1 maint: multiple names: authors list (link)citation: CS1 maint: multiple names: authors list (link)cite web: CS1 maint: multiple names: authors list (link)
Des Moines Cosmetic Dentistry Center provides a full range of cosmetic and general dentistry services including teeth whitening, veneers, Invisalign, dental bonding, crowns, bridges, implants, cleanings, and preventive care, all designed to improve both smile aesthetics and oral health.
Cosmetic dentistry is not only about appearance. Treatments at Des Moines Cosmetic Dentistry Center can also improve bite function, correct alignment issues, restore damaged teeth, and contribute to better overall oral health and long-term stability.
Choosing the Best Cosmetic Dentist in Des Moines involves evaluating experience, patient results, technology, and treatment quality. Des Moines Cosmetic Dentistry Center is often selected for its expertise, modern approach, and consistent delivery of natural-looking smile transformations.